By: Tonya Schneidereith and Fara Bowler
In Part 1 of this series, we talked about how to determine if your program is ready for simulation. In Part 2, we highlighted the role of strategic planning. Now, in Part 3, we identify different staffing models for your simulation program.
Criterion 2 of the INACSL Standard of Best Practice: SimulationSM: Operations is: “Provide personnel with appropriate expertise to support and sustain the SBE program” (INACSL Standards Committee, 2017, p. 683). So, who are responsible for supporting and sustaining your simulation program?
First, it is important to define the role of simulation personnel. Create job descriptions that align with the parent’s organizational structure. If your institution has “Clinical Educators,” “Clinical Faculty,” or “Specialty Directors,” make sure that your job titles for simulation positions use the same wording. This will help your personnel with annual evaluations, salaries, and opportunities for promotion and advancement.
Clearly identify the various roles needed for your simulation program. These can include roles for implementation, leadership, and education. Who will run the A/V equipment, service the manikins, and manage the schedule? Who will develop policies and procedures, conduct annual evaluations, and create and oversee the strategic plan? Who will develop the scenarios, implement the simulations, and facilitate the debriefing?
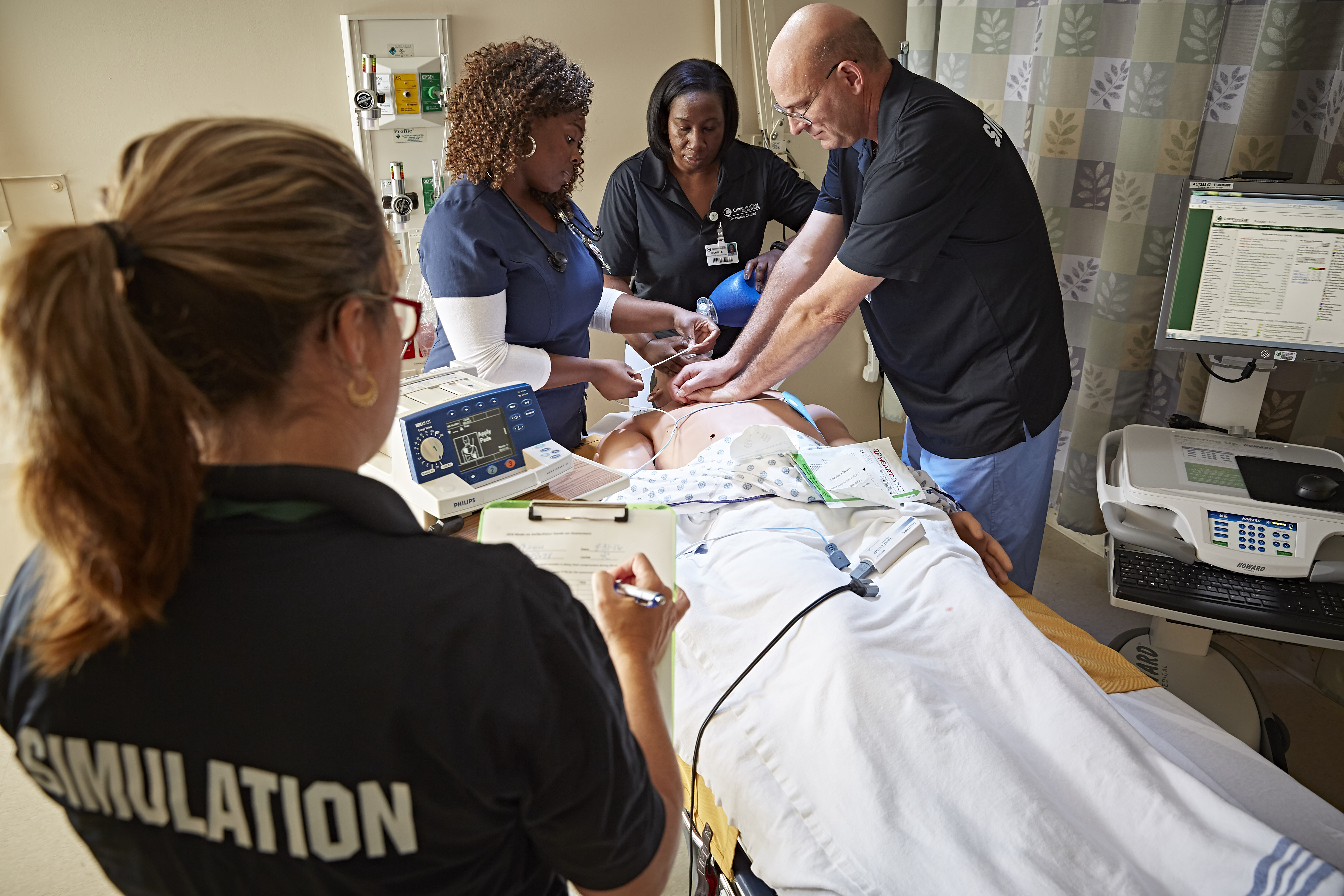
 There are multiple staffing models that can be used in simulation. These can include dedicated simulation teams, trained clinical faculty, and trained course faculty, among others. The University of Maryland School of Nursing has a dedicated simulation team that teaches only with simulation. The team consists of a director of simulation, full-time educators, part-time educators, operations specialists, and graduate teaching assistants. Clinical faculty in charge of individual clinical groups join most simulations to provide content expertise, and all simulation educators are cross-trained to facilitate the various scenarios for prelicensure and nurse practitioner courses. The implementation is organized by the operations specialists and the graduate teaching assistants. The leadership responsibilities are carried by the director of the simulation labs. The education is provided by the team members trained in simulation pedagogy.
There are multiple staffing models that can be used in simulation. These can include dedicated simulation teams, trained clinical faculty, and trained course faculty, among others. The University of Maryland School of Nursing has a dedicated simulation team that teaches only with simulation. The team consists of a director of simulation, full-time educators, part-time educators, operations specialists, and graduate teaching assistants. Clinical faculty in charge of individual clinical groups join most simulations to provide content expertise, and all simulation educators are cross-trained to facilitate the various scenarios for prelicensure and nurse practitioner courses. The implementation is organized by the operations specialists and the graduate teaching assistants. The leadership responsibilities are carried by the director of the simulation labs. The education is provided by the team members trained in simulation pedagogy.
The University of Colorado College of Nursing operational model is slightly different. Similarly, a director oversees the overarching leadership responsibilities for the program, which is also supported by three support staff: a program assistant for day-to-day operations and two simulation specialists who focus on operations. The teaching team consists of a variety of members, depending on the level of expertise needed to meet the learning outcomes of the course. The solid foundation of the teaching team is built on masters-prepared nurse faculty who are committed to ongoing faculty development in the area of simulation. The majority of their workload is dedicated to simulation pedagogy.
To support the teaching mission of the department at the University of Colorado, teaching assistants (TA) are also used, though differently than at the University of Maryland. The TAs are RNs with current clinical practice who are enrolled in a graduate program of study. They are not included in the simulation operations, but they are responsible to teach alongside the simulation faculty. For example, a TA who works in a pediatric unit and is enrolled in the pediatric nurse practitioner program will teach in the prelicensure pediatrics simulation. TAs are trained with a basic introduction to simulation and are mentored by simulation faculty. Peer-to-peer teaching has also been fostered to allow senior prelicensure students to assist juniors in basic skill acquisition. The peer mentors provide guidance in early coursework under the guidance of simulation faculty and TAs. All members of the teaching team bring their unique perspective to cultivate a well-rounded teaching model.
When trained educators aren’t available, another model for experiential learning is through outsourcing. This can be through external simulation consultants or by pairing with local hospitals or educational facilities. Consultants can come to you to design scenarios, facilitate simulations, or provide faculty development (Coppa, Schneidereith, & Farina, 2019). Alternatively, you can enter into agreements with other sites, such as community colleges, universities, or hospitals, so that your students can have simulation experiences without the institution incurring the costs of maintaining simulation space, equipment, and expert personnel.
What staffing models do you use? What advice do you have for educators who do not have the space, equipment, or personnel necessary for quality simulation experiences?
References
Coppa, D., Schneidereith, T., and Farina, C. L. (2019). Simulated home-based health care scenarios for nurse practitioner students. Clinical Simulation in Nursing, 26(1), 38-43. doi.org/10.1016/j.ecns.2018.10.002
INACSL Standards Committee. (2017). INACSL Standards of Best Practice: SimulationSM: Operations. Clinical Simulation in Nursing, 13, 681-687. doi:10.1016/j.ecns.2017.10.005


As one of the committee members who wrote this standard, I appreciate the information being shared. I would like to acknowledge my other colleagues Wendy Thomson, Teri Boese, Scott Crawford, Jesika Gavilanes, and H. Michael Young whom I worked closely with for over a year to produce these needed standards. Hopefully, people are utilizing them in conjunction with assessing their program as it relates to the SSH accreditation standards. The hope is that these standards can provide guidance on the necessary infrastructure to ensure consistency across simulation programs.